Bacteriophage
Virus defeats bacterium
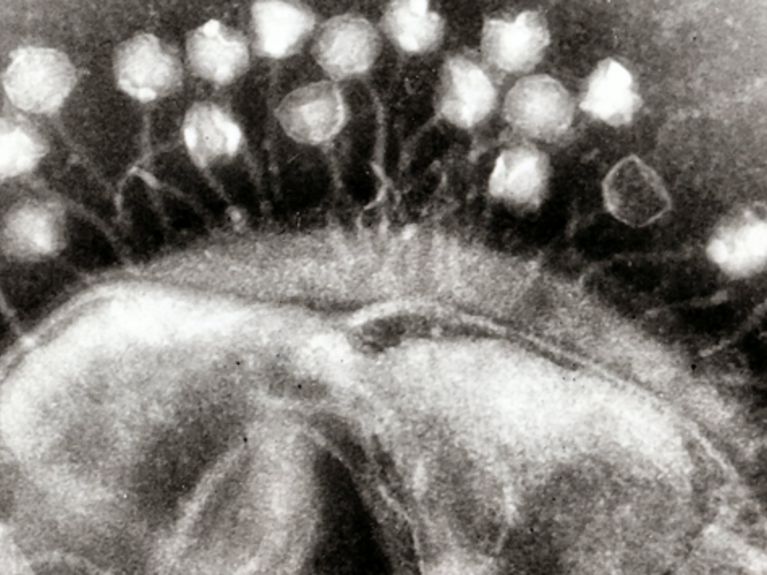
Image: Graham Beards/CC BY-SA 3.0
Bakteriophages are promising weapons in the battle against bacterial infections. But research in this area has been heretofore scarcely promoted. Thanks to several new developments, things could begin to happen in this area now.
Lung infection, urinary tract infection and infected wounds had represented a minimal threat to us for many years until recently, since they could be quickly healed through antibiotics. But this erstwhile miracle drug has been increasingly subject to failure: Some of the pathogenic bacteria have found methods in the meantime to survive these medicinal products. Susanne Häußler from the Helmholtz Centre for Infection Research in Braunschweig says: “Particularly in hospitals, germs have been developing that are resistant against many antibiotics. Here they come in contact with patients whose immune systems have already been impacted by a disease or an operation.” The physician is conducting research on Pseudomonas aeruginosa, a frequently occurring form of bacteria that, as a “hospital bug”, is capable of generating severe to fatal infections.
Antibiotics were originally natural substances, with which microorganisms in nature do battle against one another. In this context, different antibiotics produce different effects. Some of them prevent reproduction of bacteria while others kill them off by, for example, dissolving the cellular wall. But resistances emerge here in equally diverse ways: “Some bacteria have pumps with which they convey the active ingredient from the cell, others change their receptors so that the drug is not able to attach, or they directly change the antibiotic and render it ineffective,” says Häußler. In the beginning many antibiotic active ingredients were quickly discovered, but a number of them have in the meantime become ineffective; only a few new ones are being found and it takes a long time to develop them.
Given this background, bacteria’s natural enemies are once again becoming interesting: bacteriophages are viruses that are able to kill certain highly specific bacteria – and only bacteria. Their therapeutic application has enjoyed a long tradition in Eastern Europe, but here in Central Europe the respective research has long been neglected. At the Leibniz-Institute DSMZ German Collection of Microorganisms and Cell Cultures GmbH in Braunschweig there is an expert who has been tracking this phenomenon for 30 years: Christine Rohde has been involved in joint development of the phage collection there. She isolates phages from habitats such as sewage sludge, cleans them and cultivates them – always on the lookout for efficient bacteria killers. “The alluring thing about phages is that they reproduce at the source of the infection, for only as long as they are needed, after which time they disappear,” says Rohde. “They can be used externally, it is conceivable that they could be applied as inhalers against respiratory infections and strains have even been successfully administered intravenously. “
Thus far in Europe there is no legal framework for application of phages, but the approval procedure is already waiting in the starting gates. “We have compiled all of the information in Brussels – now it is in the hands of the politicians,” says Christine Rohde. “However, the respective research studies are still missing. The data at hand do not correspond to Western standards in their scope and type of survey.”
Andreas Peschel, infection biologist at the University of Tübingen, might be able to lend further momentum, through his research, to therapy with phages. He isolated protein particles, so-called lysine, from phages; these particles are sufficient to destroy bacteria. They are used to prophylactically treat staphylococci that are resistant to carriers, so that they do not disseminate the bacteria. Since lysine is able to follow the normal approval method for pharmaceuticals, it perhaps represents the final element in building the bridge to a whole phage. “Phages also have huge potential in the area of hygiene, without having to undergo the lengthy process for approval of medicinal products,” says Rohde. Breathing tubes, devices and surfaces, for example, could be effectively freed from certain dangerous bacteria by means of phages.
In addition to the search for new therapies, the key to success for Susanne Häußler lies in the support of increased diagnostics and hygiene in the clinical area. One could then become more familiar with and curb the propagation pathways of germs and reduce the use of antibiotics, says the physician: “If a patient has already had 30 contacts before it is determined whether he is carrying a multi-resistant pathogen – that is a catastrophe!” Christine Rohde wishes that comprehensive information concerning all forms of therapy would be made available to doctors, so that they could be actively involved in the discussion. She is included among the list of speakers for the healthcare summit in Berlin in October. “This is our opportunity to reach a considerably broad audience.”
Readers comments